Therapy Session
C-Gait Assessment
The C-Mill C-Gait assessment is a test to visualize the functional walking performance (or adaptation ability while walking). The C-Gait assessment is intended for all patients that are indicated for C-Mill therapy, that can walk and perform gait adaptability tasks for over 18 minutes as this assessment lasts approximately 18 minutes (depending on the patient’s speed).
The C-Gait assessment consists of 7 different tasks: visually guided stepping, tandem walking, obstacle avoidance, slalom walking, reaction to unexpected situations, speed adaptations and, if applicable, walking while performing an auditory, cognitive dual task[i].
Each task should be executed twice at different degrees of difficulty, once at an easy degree and once at a higher degree (level 2 and level 4).
Each task ends with a pop-up window containing some evaluation questions (Figure1).
The questions are:
-Rate the level of challenge
-Has the client supported oneself during the section.
-How often was the handrail used

Figure 1: Task evaluation
When the protocol is finished, all the tasks are completed, then a pop-up appears with the following questions (Figure 2):
▪ How tiring was the training? Please rate from 6-20, with 6 being ‘not tiring at all’ and 20 being ‘maximum exhaustion’.
▪ How afraid are you to fall when you walk outside? Please rate from 1-10, with 1 being ‘not afraid’ and 10 being ‘extremely afraid.

Figure 2: Final evaluation
After the assessment, the scores of each task will be presented using the spider diagram (Figure3).

Figure 3: C-Gait assessment outcome measurement
The C-Gait scores are based on the performance on each task and the difficulty level at which the task is executed (difficulty level * 2 * performance (%) / 100). Five is the highest difficulty level, but only possible to choose for the C-Gait Training[i]. The score that is displayed in the spider diagram is the highest score achieved on one of the two levels. The maximum score that can be achieved for each task in the C-Gait assessment, therefore, is eight (100% performance on level four).
[i] The C-Gait assessment has been released; however, the C-Gait training is only available for customers that participated in the C-Gait study. It won’t be developed further.
[ii] The auditory, cognitive dual task is an auditory Stroop test. The patient hears the words “low” and “high” in a certain pitch. Just like the visual Stroop test, the patient needs to say out loud whether the pitch is high or low. This task can only be performed with additional hardware and software for speech recognition. The software skips the Cognitive tasks in the C-Gait assessment because they are not available.
Functional Exercises Ideas for the RYSEN
Open the link below to read about recommendations from physiotherapists using the RYSENTM in their daily practice.
 FUNCTIONAL EXERCISES IDEAS for the RYSEN
FUNCTIONAL EXERCISES IDEAS for the RYSENC-Mill Trainer training - Theoretical test
Congratulations on completing your C-Mill training. Would you like to check your knowledge of the C-Mill? If so, please click here.
Frequently Asked Questions - General
Q: What types of training are offered?
A: Motek provides different services, for example additional or advanced training, research services or on-site support during the clinical usage of a system with patients (companionship).
For a complete overview of our services, please contact us using the contact us form at the bottom of this webpage.
Gait Offline Analysis Tool (GOAT) explained
Watch this video to find out more about how to use the GOAT for analyzing your data.
Frequently Asked Questions Gait Analysis
Q: What is the difference between anterior pelvic tilt in children and adults?
A: In a gait analysis of young children, one may see an anterior pelvic tilt of up to 20 degrees, throughout the gait cycle. Consequently one may also see a backward leaning trunk tilt of up to 20 degrees. In adults, one would usually see 0-5 degrees of anterior pelvic tilt and 5-15 degrees of forward leaning trunk tilt. These differences in measured kinematics between children and adults agree with normative data for children (Pinzone, Schwartz, Thomason, & Baker, 2014). This can be explained by the relative position of the ASIS and PSIS in children vs. adults: the PSIS are higher than the ASIS in children, which results in an anterior pelvic tilt angle.
Frequently Asked Questions GOAT
Q: I’m not able to visualize the stick figure, how is that possible?
A: In order to visualize the stick figure the kinematic and kinetic data should be reprocessed at least once in GOAT. During the reprocessing of data, the joint centers are calculated (again) in GOAT. These joint centers are needed for the stick figure. After reprocessing, save the file so reprocessing is not needed anymore.

Q: The 3D model visualization doesn’t match the marker data, is my data incorrect?
A: The Human Body Model has two separate pipelines, one for the inverse dynamics and one for the muscle visualization. Therefore, it is possible that the muscle visualization does not perfectly fit the marker data. If so, please check if the stick figure is correct. The stick figure is based on the inverse dynamics pipeline and therefore the visualization of the stick figure can give an indication whether the data is correct. If the stick figure is correct, then the kinematic, kinetic and muscle estimation data are correct and only the muscle visualization is off. If the stick figure shows a strange behavior, then the kinematic and kinetic data has the same strange behavior and then there might be something wrong with the data.
Q: The stick figure visualization doesn’t match the marker and force plate data, why?
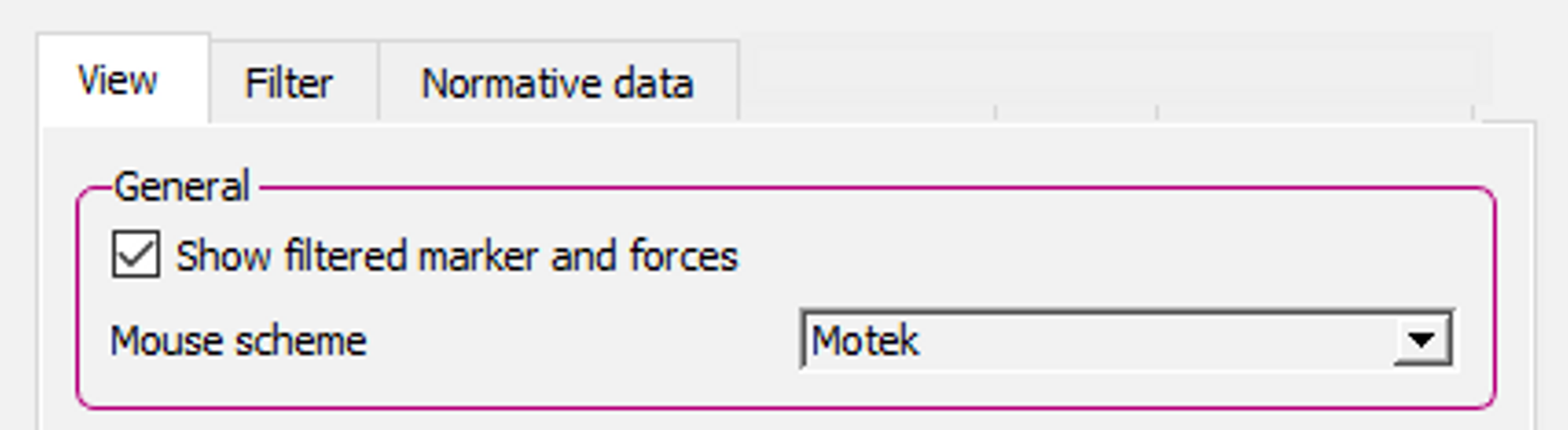
A: The stick figure is based on the joint center locations that are calculated with inverse kinematics calculation of the HBM. For these inverse kinematics calculations, filtered marker data is used. The visualization of the marker and force plate data can be filtered or unfiltered. If the stick figure visualization does not match the visualization of the marker and force plate data, the latter is probably unfiltered. This means that the checkbox: ‘Show filtered markers and forces’ is not checked. This checkbox can be found on the Menu bar: View > Settings > View and is checked by default.
Q: I don’t see any data, what could be wrong?
A: After loading a mox file, make sure that cycles are selected. When there are no cycles selected, there is no data to visualize.
Q: I see outliers in the results, what could be a reason for outliers?
A: Stepping with one foot on both belts might cause an outlier in the results of the kinetics. Outliers in the kinematics can occur if a marker is covered for a short amount of time. In the last case the calculation of the kinematics will use the last known marker position, until the marker reappears again.
Q: How can I create an overlay of previous recording in my report?
A: It is possible to create an overlay in the report which contains data of another recording of the same subject. With this overlay it is possible to compare two (or more) sessions with each other. In order to add a comparison file to the report: File | Compare | Import and select the file you wish to compare to.
Note: A file can only be added as a comparison after it is loaded and saved in GOAT at least once before the file is imported as comparison file.
Q: What do the pink, black and blue lines in the report graphs represent?
A: When a cycle is selected three lines are visible in the report graphs:
- Blue line: This is the current selected gait cycle.
- Pink vertical line: The selected frame in the cycle. This is the moment in the graph that corresponds with the current frames in the 3D window and the video window.
- Black vertical line: Toe-off of the selected cycle.
Q: Can I create and add custom norm data to a GOAT report?
A: Yes. More information can be found in the GOAT Help manual, under GOAT functionalities | Norm data.
Q: How is the stick figure created?
A: The stick figure is based on the joint center locations that are calculated by HBM. Small spheres represent the joint center locations and lines are drawn between the spheres to create the stick figure. More information about the calculations of the joint centers can be found in the HBM reference manual, which can be downloaded from the HBM tab in Post-training.
Frequently Asked Questions HBM
Q: What does HBM mean?
A: HBM stands for Human Body Model and is an inverse dynamic model to calculate joint kinematics (angles), joint kinetics (moments) and estimate muscle activity. Marker positions, measured with motion capture, and force plate data are used to calculate kinematics and kinetics. The estimation of the muscle activity is done with the joint kinematic and kinetic data in combination with assumptions of optimal voluntary muscle contractions and generalized mass properties.
Q: When do I need to calibrate HBM and when can I use reset HBM?
A: Calibration of the HBM model needs to be done in D-Flow before the first session. It is the part of the subject preparation as described in the system manual. With the HBM calibration subject-specific calibration information is saved to a T-pose file. Sometimes, during a session, the HBM calibration is lost, mostly due to occluded markers. In that case a reset of the HBM model suffices, to retrieve the HBM calibration information from the T-pose file. In short, Calibrate HBM should be done before the first session, reset HBM can be applied during a session. When a new subject arrives, a new calibration needs to be executed to write new subject-specific information to the T-pose file.
Q: How is the stick figure created?
A: The stick figure is based on the joint center locations that are calculated by HBM. Small spheres represent the joint center locations and lines are drawn between the spheres to create the stick figure. More information about the calculations of the joint centers can be found in the HBM reference manual.
Q: Can the HBM model be used for children?
A: The HBM is already being used in research for children with cerebral palsy and Duchenne’s Muscular Dystrophy in clinical gait analysis. It is also used to provide real-time feedback on kinematic and kinetic variables. When pathologies such as paralysis or spasms are involved, the outcomes of the muscle force optimization require careful attention. These precautions do not apply to the kinematic and kinetic analysis.
Q: Is there a possibility of incorporating ligament tension models (e.g., ACL, MCL) in the real-time output?
A: The existing ligament tension models are fairly simple. These could be programmed in a D-Flow expression or script module, and so provide real-time output, but this is not incorporated in HBM.
Q: What would be the difficulty in including a feature of user-defined cost functions such as muscle stress raised to a definable power exponent?
A: Professor van den Bogert has tried this, but the recurrent neural network method would not solve such a cost function quickly enough for real-time use. A different solution method would be required, which may be possible, but would definitely require more research.
Q: Is there any chance of incorporating actual EMG signals into the HBM realtime analysis?
A: In the long term, professor van den Bogert thinks this is a good idea. The CEINMS toolbox developed by David Lloyd’s group is very interesting to look at. However, currently, there are very few labs that do this, as setup requires extensive calibration. There is still a lot of research needed before this makes it into clinical practice.
Q: How does the model handle cross over between a split belt treadmill with 2 force plates?
A: The model itself assumes that correct ground reaction force data is available from both force plates. However, in our Gait Offline Analysis Tool we’ve built the ability to automatically and manually filter out gait cycles based on unexpected forces (e.g. half of the body-weight in single-stance). This is particularly useful for cross-steps on a split-belt treadmill.
Q: Can you switch off static optimisation in order to increase the rate of joint torque calculation?
A: Yes, in the MoCap module under the HBM tab there is a checkbox available called ‘Calculate muscle forces’, which switches the static optimization on and off.
Q: How are the ankle and subtalar joint axes defined?
A: Please refer to the HBM Reference Manual found in Post-Training/Software/HBM for these definitions.
Q: How accurate is the hip joint center predicted by the HBM2 model?
A: The hip joint center prediction of HBM2 is based on the regression equations of Harrington (2007). Kainz (2015) also recommends this method in his systematic review as the most accurate predictive method.
Q: I see offsets in internal/external hip rotation. How can these be influenced?
A: When using medial epicondyle markers, one of the axes used to define the femur segment is a vector through the lateral and the medial epicondyle. This means that correct marker placement of the lateral and medial epicondyle markers is vital to determine hip internal/external rotation without an offset. For example, if the medial epicondyle marker is placed anteriorly compared to the lateral epicondyle marker, this will result in a hip rotation angle which has an offset towards external rotation. When seeing an offset in internal/external hip rotation, always check the placement of the lateral and medial epicondyle markers.
Q: Double bump pattern in ankle flexion/extension moments
A: In some gait analyses, we’ve seen a clear double bump pattern in the ankle flexion/extension moments. For typically developing children, this is not what was observed in (van der Krogt, Sloot, Buizer, & Harlaar, 2015). However, typical joint kinematics associated with a pathological double dump ankle moment pattern such as excessive plantarflexion at initial contact and rapid dorsiflexion during loading response (Gage, Schwartz, Koop, & Novacheck, 2009) were not present. Examining video showed the subjects performing an early heel rise, which may explain the double bump pattern. This is also in line with (Rozumalski, Novacheck, Griffith, & Schwartz, 2014). When seeing a double bump pattern, check whether the subjects are doing an early heel rise, and whether other factors associated with a pathological double bump pattern are present.
Q: One DOF for the knee, or why we have less than three markers on the shank and thigh.
A: We often get asked why HBM does not calculate the knee internal/external rotation and abduction/adduction DOFs. Under normal conditions, the knee has very little abduction/adduction ROM. Modelling the abduction/adduction DOF would most likely reflect inherent crosstalk error in 3D kinematics calculations, rather than a true anatomical movement (Ramakrishnan & Kadaba, 1991). As for internal/external rotation, the knee does have 45 degrees of internal/external rotation ROM when flexed 90 degrees. However, HBM is mostly aimed at clinical gait analysis. During gait, the knee is largely extended, and there is little internal/external rotation ROM. So again, crosstalk would affect how well the measured angles reflect true anatomical movement. Bone pin studies showed that the soft tissue artifact for internal rotation at the knee is larger than the actual internal rotation that takes place during walking (Reinschmidt et al 1991). In summary, HBM only calculates knee flexion/extension, because the other DOFs have ROMs that are too small relative to the crosstalk error inherent in 3D kinematics. Furthermore, if three hinges were used, muscle forces would be overestimated, this problem was described nicely by Glitsch and Baumann (1997). They have shown that this is best for the analysis of muscle function and estimation of muscle forces. Users with an education in 3D kinematics are also often surprised that HBM has less than three markers on the shank and thigh. HBM can do this precisely because there is only one DOF in the knee. In most biomechanical models, each segment is modelled separately. To determine the position and orientation of a 3D segment, at least 3 markers are required. The joints between the segments then all have 6 DOF, as the segments can move independently from each other. In HBM, the position and orientation of the entire biomechanical model is determined at the same time, using global optimization. This means that HBM can also restrict joint movement to only the DOFs that make anatomical sense. HBM uses this to disallow all translational DOFs between joints, and to restrict the knee to only flexion/extension. In a sense, HBM only looks at the knee in the sagittal plane. And to calculate one angle in a 2D plane, only three markers are required: one on the top segment (thigh), one at the joint, and one at the bottom segment (shank). This allows HBM to use fewer markers on the thigh and shank than other biomechanical models.
Q: How precise models HBM2 the trunk internal/external rotation?
A: Normative literature on trunk kinematics is not readily available, due to there not being a standard model for trunk kinematics. However, Leardini et al. compared eight different trunk models, of which one is the ISB trunk model (Leardini, Biagi, Belvedere, & Benedetti, 2009). The trunk model in HBM2 uses almost the same marker set as the ISB trunk model, the only difference is using T10 vs. using T8. The trunk tilt and lateroflexion found in HBM2 shows a similar pattern to the pattern seen in Leardini et al. Trunk internal/external rotation however is slightly different: in HBM2, peak rotation is at 10% of the gait cycle, whereas Leardini et al. see the peak rotation exactly at initial contact. Otherwise the pattern is similar. It’s hard to say which one best models the true trunk rotation, but both will be a simplification of the true movement of the trunk, since both consider the trunk as a single segment.
Q: Please explain the toe joint center
A: HBM has a toe joint, which is used in the kinematic analysis, but this toe joint should probably be removed in future versions. The existence of the toe joint is for historical reasons: when HBM was first developed, the kinematic analysis was also used for the visualization. It would have looked bad to have a completely rigid foot. However, the visualization currently uses its own skeleton, so this no longer applies. Also, although the toe joint is used in the kinematic analysis, it is not used in the muscle modeling or the inverse dynamics. This is because a force plate cannot distinguish between force applied at the foot and force applied at the toe. So the only function the toe joint served (the visualization) no longer applies, and it can be safely removed. A reason to do the work to remove the toe joint is that when HBM joints are used as input for an OpenSim model (as in MD-PAEDIGREE), the place of the HBM toe joint results in an anatomically incorrect foot. This is because the HBM toe joint is placed 6 centimeters behind the CM2 marker, which is anatomically incorrect, but necessary to prevent problems in the inverse kinematic solver. Removing the toe joint would prevent propagating this anatomically incorrect toe joint to a derived OpenSim model.
Therapy Goals Quicksheet
This document shows which applications are suitable for training which specific therapy goals.
 Therapy Goals Quicksheet
Therapy Goals QuicksheetGRAIL - Handling Emergency Situations
This document describes how to handle emergency situations during a GRAIL treatment or analysis session.
 Handling Emergency Situations
Handling Emergency SituationsTherapy Goals
This document provides a quick overview on all training categroies of the C-Mill and their corresponding treatment goals.
 Quick Sheet - Therapy Goals
Quick Sheet - Therapy GoalsTherapy Guide
This guideline describes the clinical workflow on the C-mill system and explains the different categories Stand, Step and Walk with their corresponding treatment goals, assessments and training for patients with balance and walking impairments.
 C-Mill Therapy Guide
C-Mill Therapy GuideC-Mill Assessment Questions
Q: Is the width between the projected steps, that are projected onto the belt for standing balance applications and assessments, specific for each patient?
A: Yes. The width between the projected feet is based on the length of the patient.
Q: Why is there no score for the cognitive dual task of the C-Gait assessment?
A: The cognitive dual task requires additional hardware (a special headset). The patient needs to indicate if the words ‘high’ and ‘low’ are spoken with a high or low pitch.
Q: Is a harness required during the execution of a balance assessment?
A: Yes, a patient should always wear a safety harness, that is attached to a safety portal via a safety line.
Q: What can be deducted from the shape of the butterfly?
A: The butterfly can visualize relative differences between left and right steps, or difficulties in weight assumption from one leg to the other. Furthermore, it can visualize step width and gait asymmetries. Absolute values for step length cannot be visualized with the butterfly, because the butterfly reflects the CoP (Center of Pressure) trajectory on the belt surface and this is also depended on the treadmill speed.
C-Mill CueFors Questions
Q: Track images: some images can only have a positive or negative score. What is the underlying logic per image?
A: Cues can only have a positive score. Animals can both have a negative as well as positive score and obstacles can only have a negative score.
Q: How are the default width and height of the stepping stones/ obstacles determined? And where can I find the exact dimensions?
A: The width and height are based on the foot dimensions that need to be stored for each patient/subject in the database. The exact dimensions of the stepping stones or obstacles can be seen in the CUEING.csv file, which is created when the measurement is exported.
C-Mill General Questions
Q: What types of training/services/support does Motek provide?
A: Motek provides different services, for example additional or advanced training, research services or on-site support during the clinical usage of a system with patients (companionship). We can also consult you during the implementation phase of your system or share experiences regarding reimbursement.
For a complete overview of our services, please send an email to clinical.applications@motekforcelink.com.
Q: Where can I find other centers to exchange experiences?
A: Please contact us via clinical.applications@motekforcelink.com and we will try to put you into contact with other centers. If applicable, please describe the specific characteristics/requirements of the centers you are looking for.